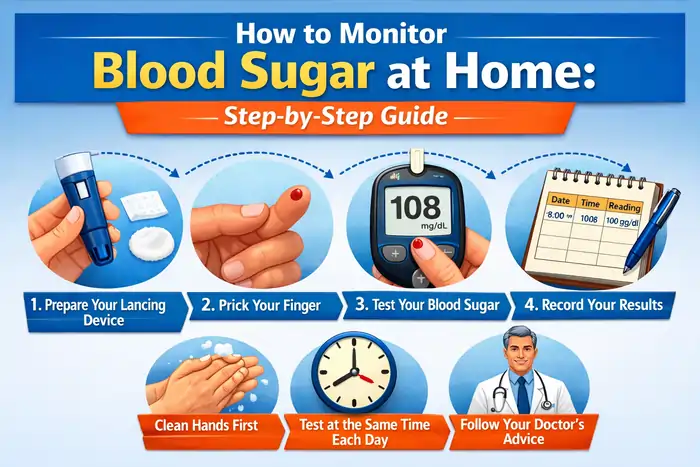
Monitoring blood sugar at home is one of the most important self-management skills for people living with diabetes because it shows how your daily choices affect glucose and helps you and your care team adjust treatment safely. Clinical guidance such as the American Diabetes Association (ADA) Standards of Medical Care in Diabetes highlights self-monitoring of blood glucose (SMBG) as a key tool for improving glycemic control and guiding medication changes, a message echoed in ADA’s patient-facing overview on checking your blood glucose.
Why Monitoring Blood Sugar at Home Matters
Diabetes is a chronic condition characterized by elevated blood glucose due to problems with insulin production, insulin action, or both, and the World Health Organization notes that poorly controlled diabetes increases the risk of blindness, kidney failure, heart disease, stroke, and lower limb amputation in its diabetes fact sheet. Home monitoring helps you detect hyperglycemia (high blood sugar) and hypoglycemia (low blood sugar), guide medication dosing (especially insulin), evaluate how food and activity affect your levels, and reduce the risk of long-term complications.
If diabetes is not properly monitored, complications may develop silently; our guide on uncontrolled diabetes and complications explains these risks in more detail.
If you are newly diagnosed or reviewing your care plan, it can help to revisit our overview of type 2 diabetes: prevention, monitoring, and complications.
Who Should Monitor Blood Sugar at Home?
The ADA recommends individualized monitoring frequency based on treatment and risk, but SMBG is especially important for people using insulin, those with frequent hypoglycemia, pregnant women with diabetes, anyone actively adjusting medications, and patients with poorly controlled diabetes. People with newly diagnosed type 2 diabetes may also benefit from home monitoring to understand patterns and treatment response, a point reinforced in NIDDK’s guidance on managing diabetes and checking blood glucose at home.
If you are unsure whether you have symptoms that warrant testing, you can review our checklist of early warning signs of diabetes.
Methods of Monitoring Blood Sugar at Home
There are two primary methods:
- Glucometer (fingerstick testing)
- Continuous Glucose Monitoring (CGM)
Both methods are recognized in ADA care guidelines and in practical summaries on SMBG and CGM use for day-to-day diabetes management.
Method 1: How to Use a Glucometer (Step-by-Step)
A glucometer measures blood glucose using a small drop of blood from your fingertip.
What you need
- Glucose meter
- Test strips
- Lancet device
- Lancets
- Alcohol swab (optional)
- Logbook or digital app
Step-by-Step Instructions
Step 1: Wash and dry your hands
Clean hands help prevent inaccurate readings, and soap and water are preferred over alcohol when possible; the CDC’s handwashing guidance stresses proper washing technique before health-related procedures.
Step 2: Insert test strip into meter
Insert a new test strip according to the meter manufacturer’s instructions.
Step 3: Prepare the lancet device
Insert a new sterile lancet and adjust the depth if needed.
Step 4: Prick the side of your fingertip
Use the side of the fingertip rather than the pad to reduce discomfort.
Step 5: Apply blood to test strip
Touch the test strip to the blood drop; the meter will display your glucose level within seconds.
Step 6: Record the reading
Track the date, time, glucose value, whether it was fasting, pre-meal, or post-meal, and any symptoms. Clinical articles on SMBG emphasize that recognizing patterns over time is more important than focusing on a single number.
When Should You Check Blood Sugar?
The ADA suggests individualized testing schedules, but common times include before meals, 2 hours after meals, before bedtime, before exercise, and whenever you feel symptoms of high or low blood sugar. For people on intensive insulin regimens, ADA guidance recommends checking multiple times per day — often before meals and snacks, at bedtime, before exercise, and when hypoglycemia is suspected.
Understanding Target Blood Sugar Levels
Target ranges vary depending on age, pregnancy status, comorbidities, and overall health. ADA standards for many nonpregnant adults often use:
- Fasting (before meals): roughly 80–130 mg/dL
- About 2 hours after meals: typically under 180 mg/dL
These figures are reflected in ADA’s professional standards and patient guidance, with the understanding that your provider may individualize them.
What Is HbA1c and Why It Matters
HbA1c reflects average blood glucose over the past 2–3 months. ADA guidance recommends testing at least twice yearly in stable patients, and up to four times per year in those whose therapy is changing or who are not meeting goals. Many adults aim for an HbA1c around under 7%, but this is individualized based on age, comorbidities, and risk of hypoglycemia. Home monitoring complements HbA1c by showing day-to-day fluctuations and hypoglycemia that an average alone can miss.c
Method 2: Continuous Glucose Monitoring (CGM)
CGM systems measure glucose levels in interstitial fluid every few minutes via a sensor placed under the skin.
Benefits include:
- Real-time glucose tracking
- Alerts for high or low glucose
- Trend arrows and graphs
- Fewer fingersticks in many systems
The ADA recognizes CGM as especially beneficial for people using insulin and those at high risk of hypoglycemia, and updated Standards sections on “Blood Glucose Monitoring” highlight its growing role in type 2 diabetes as well.professional.
Signs of High and Low Blood Sugar
Signs of high blood sugar (hyperglycemia) may include increased thirst, frequent urination, fatigue, and blurred vision. If these persist, consult your provider; our guide on early warning signs of diabetes explains these symptoms in more detail.
Signs of low blood sugar (hypoglycemia) include shakiness, sweating, dizziness, confusion, and rapid heartbeat; severe hypoglycemia is an emergency and requires immediate treatment.
Common Mistakes in Home Blood Sugar Monitoring
Common pitfalls include:
- Not washing hands before testing
- Using expired or improperly stored test strips
- Not calibrating the meter if required
- Squeezing the finger excessively (which can dilute the sample)
- Failing to record readings or share them with your care team
Reviews on SMBG stress that training and consistent technique are essential to interpret readings correctly and avoid mismanagement.
How Food, Exercise, Stress, and Illness Affect Blood Sugar
Food:
Carbohydrates have the biggest and fastest impact on blood sugar. Tracking post-meal readings helps you learn which foods spike glucose, how portion sizes affect you, and when your peaks occur. The CDC’s advice on eating well with diabetes underscores how meal choices and timing influence glucose patterns.
Exercise:
Physical activity increases insulin sensitivity and can lower blood sugar and improve glucose utilization, although intense exercise may temporarily raise glucose in some people. Monitoring before and after new exercise routines helps you understand your own response.
Stress and illness:
Stress hormones can raise glucose, and during illness, blood sugar often runs higher, so monitoring frequency should increase and hydration is crucial. These “sick day” adjustments are a standard part of diabetes self-management education.
When to Contact Your Healthcare Provider
Seek medical advice if:
- Fasting readings remain consistently above your target
- You experience frequent hypoglycemia
- Blood sugar readings are persistently very high (for example, around or above 300 mg/dL)
- You feel confused, very drowsy, or otherwise severely unwell
Uncontrolled glucose over time damages kidneys, eyes, heart, and nerves, and the CDC identifies diabetes as a leading cause of kidney failure and blindness in its overview of diabetes complications. Routine monitoring reduces these risks by enabling timely medication and lifestyle adjustments.
Creating a Monitoring Routine
Successful monitoring includes:
- Fixed testing times that fit your treatment plan
- Logging results in a notebook or app
- Reviewing patterns weekly (for example, fasting trends or post-meal spikes)
- Bringing logs or CGM reports to appointments
NIDDK and ADA both emphasize that SMBG works best when readings are used to adjust diet, activity, and medication in partnership with your healthcare team, not just collected and ignored.
Frequently Asked Questions
How often should I check my blood sugar?
Frequency depends on your treatment plan. People on multiple daily insulin injections or pumps typically check several times per day, while those on non-insulin regimens may check less often but still benefit from periodic monitoring around meals and activity, as described in ADA recommendations on SMBG.
Can I rely only on HbA1c?
No. HbA1c shows an average but does not reveal daily swings, hypoglycemia episodes, or how specific meals and activities affect your levels. Combining HbA1c with home monitoring provides a fuller picture of control.
Is CGM better than fingersticks?
CGM offers continuous data, alerts, and trends, which can be especially helpful for those on insulin or with frequent lows, but some devices still require confirmatory fingersticks in certain situations. Cost, insurance coverage, and personal preference also play roles in choosing between CGM and traditional meters.
Final Thoughts
Monitoring blood sugar at home is a powerful tool in diabetes management. It provides immediate feedback, supports safer medication adjustments, and helps prevent serious complications when combined with professional care and lifestyle changes. With structured monitoring, individualized targets, and evidence-based treatment, many people with diabetes significantly reduce long-term health risks and live full, active lives.
If you suspect early symptoms or have questions about your monitoring routine, discuss them with your healthcare provider so you can tailor a plan that fits your daily life and medical needs.
⚠️ Medical Disclaimer
The information provided on MedEduHub is for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. If you experience severe hyperglycemia, confusion, vomiting, chest pain, trouble breathing, or other signs of a medical emergency, seek immediate medical care. Always consult a licensed healthcare provider before starting, stopping, or changing any diabetes treatment or blood sugar monitoring plan.
👩⚕️ Written by: Eden Grace Ramos-Arsenio, RN
📚 Medical Sources & References
This article is based on current clinical guidelines and peer-reviewed research from the American Diabetes Association Standards of Care and blood glucose monitoring guidance, CDC diabetes management resources on managing and monitoring blood sugar, the WHO diabetes fact sheet, the National Institute of Diabetes and Digestive and Kidney Diseases guidance on managing diabetes at home, and American Heart Association information on diabetes complications and cardiovascular risk.

