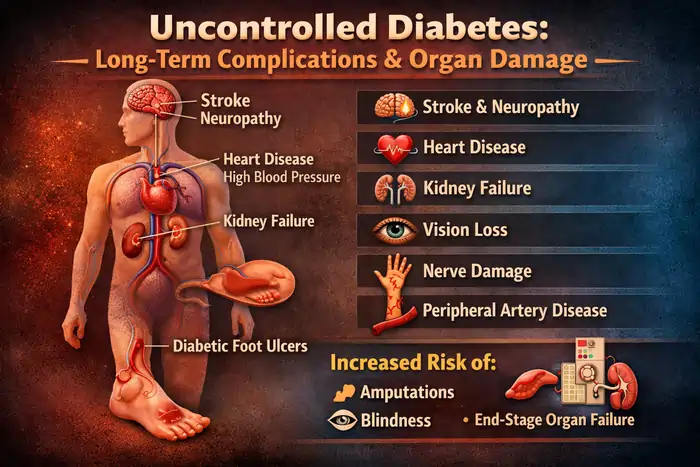
Diabetes is a chronic metabolic disorder characterized by persistently elevated blood glucose levels resulting from impaired insulin production, insulin resistance, or both. When blood sugar remains poorly controlled over time, it can cause widespread damage to blood vessels, nerves, and major organs throughout the body. The World Health Organization notes that diabetes is a leading cause of blindness, kidney failure, heart attacks, stroke, and lower-limb amputation worldwide in its diabetes fact sheet.
The Centers for Disease Control and Prevention also reports that uncontrolled diabetes significantly increases the risk of serious health problems affecting the heart, kidneys, eyes, and nervous system in its overview of diabetes complications. Understanding how uncontrolled diabetes affects the body helps patients recognize the importance of early detection, consistent monitoring, and proper treatment.
If you are newly diagnosed or reviewing your care plan, you may want to revisit our comprehensive guide on type 2 diabetes: prevention, monitoring, and complications.
Why High Blood Sugar Causes Organ Damage
When glucose levels remain elevated for months or years, several biological processes contribute to tissue damage. High blood sugar can damage small blood vessels (microvascular damage), damage large arteries (macrovascular disease), increase inflammation, promote oxidative stress, and interfere with normal nerve function. NIDDK explains that prolonged hyperglycemia injures blood vessel walls and reduces circulation to vital organs, leading to many of the complications associated with diabetes, in its guidance on preventing diabetes problems.
Because this damage often occurs gradually, individuals may not notice symptoms until complications have already developed. Monitoring glucose regularly is one of the most effective ways to prevent these outcomes; if you are unsure how to do this safely, review our step-by-step guide on how to monitor blood sugar at home.
Cardiovascular Disease and Diabetes
Cardiovascular disease is the leading cause of death among people with diabetes. The American Heart Association notes that adults with diabetes are significantly more likely to develop heart disease or experience a stroke compared with individuals without diabetes in its section on diabetes and cardiovascular risk.
Elevated blood glucose contributes to artery inflammation, plaque formation, reduced blood vessel elasticity, and increased blood clot risk, all of which accelerate atherosclerosis. Common cardiovascular complications include coronary artery disease, heart attack, stroke, and peripheral artery disease, and the CDC highlights that diabetes approximately doubles the risk of heart disease and stroke in its guidance on how to put the brakes on diabetes complications.
Symptoms of cardiovascular complications may include chest pain, shortness of breath, leg pain when walking, or sudden weakness or numbness, and any of these warrant urgent medical evaluation. Preventive strategies include blood sugar control, cholesterol management, blood pressure monitoring, smoking cessation, and healthy lifestyle habits, as reinforced across prevention resources from WHO, CDC, and professional societies.
Diabetic Neuropathy (Nerve Damage)
Diabetic neuropathy refers to nerve damage caused by chronic high blood glucose. NIDDK identifies diabetic neuropathy as one of the most common complications of long-term uncontrolled diabetes in its overview of nerve damage and diabetic neuropathies.
There are several forms of diabetic neuropathy:
Peripheral Neuropathy
Peripheral neuropathy is the most common type and affects the hands and feet. Symptoms may include tingling, burning pain, numbness, increased sensitivity, and muscle weakness, and loss of sensation in the feet increases the risk of injury and infection because minor wounds may go unnoticed.
Autonomic Neuropathy
Autonomic nerve damage affects internal organs. Possible symptoms include digestive problems, abnormal sweating, bladder dysfunction, and blood pressure instability, all of which NIDDK links to autonomic nerve involvement in its neuropathy resources.
Proximal and Focal Neuropathy
Proximal neuropathy affects the hips, thighs, or buttocks and can cause severe pain and muscle weakness, while focal neuropathy involves sudden nerve damage in specific areas such as the eye muscles or face. Tight blood sugar control, blood pressure management, and early symptom reporting help reduce the risk and slow progression.
Diabetic Nephropathy (Kidney Disease)
Diabetic nephropathy is kidney damage caused by chronic high blood glucose. The National Kidney Foundation and other kidney health organizations note that diabetes is the leading cause of chronic kidney disease and kidney failure in many countries, a pattern also highlighted in WHO’s diabetes fact sheet.
High blood sugar damages tiny filtering units in the kidneys called glomeruli. Over time this leads to protein leakage into urine (albuminuria), reduced kidney function, fluid retention, and high blood pressure. Advanced kidney disease may require dialysis or kidney transplantation.
Routine screening is essential; ADA Standards of Care recommend annual urine albumin testing for individuals with diabetes so that early diabetic kidney disease can be detected and treated. Early detection allows interventions such as blood pressure control, ACE inhibitors or ARBs, and improved glycemic management to slow disease progression.
Diabetic Retinopathy (Vision Loss)
Diabetic retinopathy is damage to the blood vessels of the retina. The National Eye Institute explains that diabetic retinopathy is a leading cause of blindness among adults in its educational pages on diabetic retinopathy and diabetic eye disease.
High blood sugar damages small blood vessels in the retina, leading to swelling, leakage, and abnormal blood vessel growth. Early stages may not cause symptoms, which is why regular screening is critical. As the condition progresses, patients may experience blurred vision, floaters, dark spots in vision, or vision loss.
Annual dilated eye exams are recommended for people with diabetes so ophthalmologists can detect retinopathy early and apply treatments such as laser therapy, injections, or surgery when indicated.
Diabetic Foot Complications
Nerve damage combined with poor circulation can lead to serious foot complications. Common issues include foot ulcers, skin infections, and delayed wound healing. The CDC reports that diabetes is a leading cause of non-traumatic lower limb amputations worldwide in its feature on diabetes and amputations.
Loss of sensation in the feet may prevent individuals from noticing injuries, while poor blood flow slows healing and increases infection risk. Preventive care includes daily foot inspection, proper footwear, prompt treatment of wounds, and routine podiatry care, all of which are core recommendations in multidisciplinary foot care programs for people with diabetes.
Diabetic Gastroparesis
Gastroparesis is a condition in which nerve damage slows stomach emptying. NIDDK describes gastroparesis as a complication of long-term diabetes affecting digestive function in its resource on gastroparesis and diabetes.
Symptoms include nausea, vomiting, bloating, early satiety, and unpredictable blood sugar fluctuations due to delayed absorption. Managing blood glucose carefully, adjusting meal timing and composition, and using medications when indicated can help reduce symptom severity.
Mental Health and Diabetes
Living with uncontrolled diabetes can also affect mental health. Research shows increased risk of depression, anxiety, and diabetes distress in people with diabetes compared with the general population. The CDC highlights the psychological burden of diabetes management and the importance of emotional support in its page on mental health and diabetes.
Mental health challenges may make self-management more difficult, which can worsen glycemic control and create a vicious cycle. Integrated care approaches that address both physical and psychological health—such as involving behavioral health, diabetes education, and social support—are recommended.
The Role of Blood Sugar Monitoring
Regular blood glucose monitoring helps detect patterns that may lead to complications. Monitoring allows individuals to identify high blood sugar early, adjust medications or diet, and prevent dangerous glucose fluctuations, a strategy strongly supported by ADA and NIDDK self-management resources.professional.diabetes+1
For detailed, practical instructions, you can follow our guide on how to monitor blood sugar at home.
Recognizing Early Warning Signs
Many complications develop after years of uncontrolled glucose. However, early symptoms of diabetes may include increased thirst, frequent urination, fatigue, blurred vision, and slow wound healing, which both CDC and NIDDK list as classic signs in their pages on diabetes symptoms and diabetes symptoms and causes.
Recognizing these symptoms early allows timely diagnosis and treatment. For a full checklist, visit our article on early warning signs of diabetes.
Preventing Diabetes Complications
Evidence shows that maintaining blood glucose within target range significantly reduces complications. Long-term studies and guideline summaries emphasize that tight but safe glycemic control, combined with blood pressure and lipid management, dramatically lowers rates of eye, kidney, and nerve disease as well as cardiovascular events.
Key strategies include:
- Regular monitoring: Tracking blood glucose levels helps identify trends and prevent severe highs or lows.
- Medication adherence: Taking prescribed medications consistently helps maintain stable glucose levels.
- Healthy diet: Balanced meals with controlled carbohydrate intake help prevent glucose spikes.
- Physical activity: Regular exercise improves insulin sensitivity and cardiovascular health.
- Routine medical checkups: Screenings such as eye exams, kidney function tests, foot examinations, and cholesterol testing allow early detection of complications.
When to Seek Medical Attention
Contact your healthcare provider if you experience persistently high blood glucose readings, severe fatigue, vision changes, numbness in the feet, or chest pain and shortness of breath. CDC and AHA resources both stress that these may be early signs of serious complications like heart disease, neuropathy, or retinopathy.heart+1
Seek emergency medical care if you experience confusion, difficulty breathing, severe dehydration, or loss of consciousness, as these may indicate acute metabolic emergencies such as diabetic ketoacidosis or hyperosmolar crisis.
Frequently Asked Questions
What happens if diabetes remains uncontrolled for many years?
Chronic high blood glucose can damage the heart, kidneys, eyes, nerves, and blood vessels, increasing the risk of life-threatening complications such as heart attack, stroke, kidney failure, blindness, and amputations, as summarized by WHO, CDC, and the International Diabetes Federation in their sections on diabetes complications.
Can diabetes complications be reversed?
Some early complications may improve if blood sugar control, blood pressure, and cholesterol are optimized, but many advanced complications (such as established kidney failure or severe retinopathy) are difficult or impossible to fully reverse, which is why early prevention and treatment are so heavily emphasized in guidelines.
How long does it take for complications to develop?
Complications typically develop over years of uncontrolled diabetes, though the timeline varies based on genetics, duration of disease, and control of risk factors. Some microvascular changes can begin within a few years of diagnosis if blood sugars remain high.
Can monitoring blood sugar prevent complications?
Yes. Regular monitoring allows early detection of abnormal levels and helps guide treatment decisions that reduce complication risk; ADA and NIDDK both position blood glucose monitoring as a cornerstone of diabetes self-management and complication prevention.
Is it possible to live a healthy life with diabetes?
With proper management—routine monitoring, medication adherence, healthy diet, physical activity, and regular follow-up—many individuals with diabetes live long, healthy lives and prevent or significantly delay complications, as underscored in WHO and CDC messaging on living well with diabetes.
Final Thoughts
Uncontrolled diabetes can have serious long-term consequences affecting nearly every organ system in the body, yet global data consistently show that these complications are largely preventable through early diagnosis, consistent monitoring, healthy lifestyle habits, and evidence-based medical care. Understanding how diabetes affects the body empowers individuals to take proactive steps toward better health and improved quality of life.
If you have diabetes or are at risk, regular communication with your healthcare provider and ongoing self-management are essential.
⚠️ Medical Disclaimer
The information provided on MedEduHub is for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. If you experience severe hyperglycemia, confusion, chest pain, breathing difficulty, or signs of a medical emergency, seek immediate medical attention. Always consult a licensed healthcare provider before starting, stopping, or changing any diabetes treatment plan.
👩⚕️ Written by: Eden Grace Ramos-Arsenio, RN
Registered Nurse | Clinical Health Educator
📚 Medical Sources & References
This article is based on current clinical guidelines and peer-reviewed research from the WHO diabetes fact sheet, CDC diabetes complications resources, the American Diabetes Association Standards of Medical Care in Diabetes, the National Institute of Diabetes and Digestive and Kidney Diseases, National Eye Institute diabetic eye disease resources, and American Heart Association guidance on diabetes complications and cardiovascular risk.professional.

