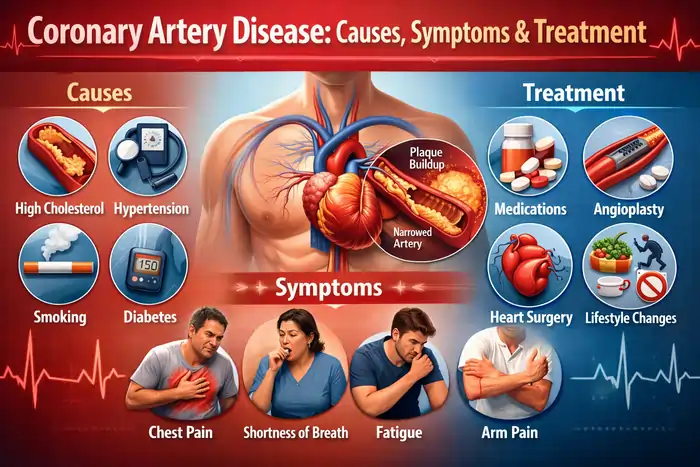
Coronary artery disease (CAD) is one of the most common forms of cardiovascular disease and a leading cause of death worldwide, because it narrows or blocks the coronary arteries that supply oxygen-rich blood to the heart muscle. The World Health Organization notes that cardiovascular diseases are the leading cause of death globally, responsible for nearly 18 million deaths each year, with coronary artery disease as a major contributor in its cardiovascular disease fact sheet. In the United States, the Centers for Disease Control and Prevention reports that coronary heart disease is the most common type of heart disease and accounts for hundreds of thousands of deaths annually in its heart disease overview.
Coronary artery disease develops gradually over time and may remain silent for years before symptoms appear. However, early recognition and proper management can significantly reduce the risk of serious complications such as heart attacks. If you would like a broader overview of cardiovascular health, you can connect this article to your pillar guide on heart disease risk factors, symptoms, and prevention by linking phrases like “broader overview of cardiovascular health” or “how different cardiovascular conditions develop” to that main resource.
What Is Coronary Artery Disease?
Coronary artery disease occurs when fatty deposits called plaques accumulate inside the coronary arteries, which supply oxygen and nutrients to the heart muscle. As plaque builds up, the arteries become narrowed and stiff, reducing blood flow to the heart in a process known as atherosclerosis. The U.S. National Heart, Lung, and Blood Institute explains that atherosclerosis develops when cholesterol, fats, and other substances accumulate along artery walls and eventually restrict blood flow in its overview of atherosclerosis.
When coronary arteries cannot deliver enough oxygen-rich blood to the heart, symptoms such as chest pain may occur, and if an artery becomes completely blocked, it can result in a heart attack. When you mention “warning signs of this medical emergency,” you can naturally link that phrase to your dedicated guide on signs of a heart attack, which explains symptoms and when to seek urgent medical care.
How Coronary Artery Disease Develops
Coronary artery disease usually develops slowly over decades. The process often begins with damage to the inner lining of the arteries; over time, plaque accumulates and causes narrowing. Several biological processes contribute, including inflammation inside artery walls, cholesterol accumulation, oxidative stress, and abnormal blood clot formation. The American Heart Association explains that these processes gradually reduce blood flow and increase the risk of heart attack and stroke in its education about cholesterol and atherosclerosis.
As plaques enlarge, they may become unstable, rupture, and lead to blood clots that abruptly block the artery, triggering a heart attack.
Symptoms of Coronary Artery Disease
In early stages, coronary artery disease may not cause noticeable symptoms. As artery narrowing becomes more severe, symptoms often appear during physical exertion or emotional stress, when the heart needs more oxygen. Common symptoms include chest pain or pressure (angina), shortness of breath, fatigue, dizziness, pain in the neck, jaw, or arm, and nausea. The CDC notes that chest discomfort or pressure is one of the most common symptoms of reduced blood flow to the heart in its section on heart disease symptoms.
Angina: A Common Symptom of CAD
Angina is a type of chest pain caused by reduced blood flow to the heart muscle. It may feel like pressure, squeezing, heaviness, or burning in the chest and typically occurs during exercise, stress, heavy meals, or exposure to cold weather. The American Heart Association explains that angina symptoms often improve with rest or medication in its overview of angina. However, persistent, severe, or worsening chest pain should always be evaluated promptly by a healthcare provider.
Major Risk Factors for Coronary Artery Disease
Several risk factors increase the likelihood of developing CAD. Some are modifiable—meaning lifestyle changes can reduce risk—while others, such as age and family history, cannot be changed. The CDC lists high blood pressure, high cholesterol, smoking, diabetes, obesity, physical inactivity, unhealthy diet, family history of heart disease, and older age among the major risk factors in its page on heart disease risk factors.
- High cholesterol: Elevated LDL (“bad”) cholesterol contributes to plaque formation inside arteries and over time narrows coronary arteries. The American Heart Association recommends routine cholesterol screening and heart-healthy lifestyle changes in its cholesterol resources.
- High blood pressure: Hypertension damages artery walls and accelerates plaque buildup; the CDC identifies it as one of the strongest risk factors for heart disease and stroke in its overview of high blood pressure.
- Smoking: Tobacco smoke injures blood vessels and promotes inflammation. The World Health Organization identifies tobacco use as a major preventable cause of cardiovascular disease in its tobacco fact sheet, and even secondhand smoke increases cardiovascular risk.
- Diabetes: People with diabetes have a higher likelihood of CAD because elevated blood glucose damages blood vessels and accelerates atherosclerosis. The CDC notes that adults with diabetes are nearly twice as likely to develop heart disease in its feature on diabetes and heart disease.
- Obesity and physical inactivity: Excess body weight and sedentary lifestyle contribute to high blood pressure, abnormal cholesterol, and insulin resistance. Regular physical activity improves circulation and reduces inflammation; the American Heart Association recommends at least 150 minutes per week of moderate exercise in its fitness recommendations.
How Coronary Artery Disease Is Diagnosed
Doctors diagnose CAD using a combination of medical history, physical examination, and diagnostic testing. Common tests include:
- Electrocardiogram (ECG): Measures the electrical activity of the heart and can show prior or ongoing damage.
- Stress testing: Assesses how the heart performs under physical stress, often using a treadmill or medication to increase heart workload.
- Echocardiogram: Uses ultrasound to visualize heart structure and function.
- Coronary angiography: Uses contrast dye and X-rays to identify blocked or narrowed coronary arteries.
The National Heart, Lung, and Blood Institute notes that these tests help clinicians detect CAD and decide on the best treatment approach in its information on coronary heart disease diagnosis and management.
Treatment Options for Coronary Artery Disease
Treatment depends on the severity of the disease and the patient’s overall health but usually includes a combination of lifestyle changes, medications, and sometimes procedures.
Lifestyle Changes
Lifestyle modification is the first step in managing CAD. Important changes include a heart-healthy diet, regular exercise, quitting smoking, weight management, and stress reduction. You can naturally link phrases like “lowering cardiovascular risk” or “how daily habits influence heart health” to your prevention-focused guide on lowering cardiovascular risk, which gives practical strategies for diet, movement, and routines.
Medications
Doctors may prescribe:
- Statins to lower cholesterol
- Beta blockers to reduce heart workload and control heart rate
- ACE inhibitors or ARBs to lower blood pressure and protect the heart
- Antiplatelet medications such as aspirin to reduce blood clot risk
These medications help prevent heart attacks and improve long-term outcomes when combined with lifestyle changes, as reflected in guideline summaries from major cardiology organizations.
Medical Procedures
When artery narrowing becomes severe or symptoms persist despite medications, procedures may be needed:
- Angioplasty: A balloon is used to open narrowed arteries.
- Stent placement: A small mesh tube is inserted to keep the artery open.
- Coronary artery bypass surgery: Surgeons create new pathways for blood to reach heart muscle by bypassing blocked arteries.
The American Heart Association describes these procedures as effective ways to restore blood flow in patients with significant CAD in its coronary artery disease and treatment resources.
Complications of Coronary Artery Disease
If left untreated, CAD can lead to serious complications including heart attack, heart failure, arrhythmias, and sudden cardiac arrest. The WHO emphasizes that cardiovascular complications like these remain a major cause of global mortality in its cardiovascular disease fact sheet, which underscores the importance of early detection and treatment.
Preventing Coronary Artery Disease
Many cases of coronary artery disease are preventable. Prevention focuses on reducing risk factors through healthy diet, regular physical activity, smoking cessation, blood pressure and cholesterol control, and effective diabetes management. A Mediterranean-style diet rich in fruits, vegetables, whole grains, and healthy fats has been widely recommended for cardiovascular protection, and the American Heart Association highlights heart-healthy eating patterns as a key prevention tool in its healthy eating guidance. Your internal article on lowering cardiovascular risk fits well wherever you discuss long-term lifestyle prevention.
The Importance of Regular Heart Health Screenings
Regular health checkups help identify risk factors before symptoms appear. Recommended screenings include blood pressure measurement, cholesterol testing, blood glucose testing, and weight or BMI monitoring. The CDC emphasizes that early detection of cardiovascular risk factors significantly reduces the likelihood of heart disease in its prevention-focused page on heart disease prevention.
Frequently Asked Questions
What is coronary artery disease?
Coronary artery disease occurs when plaque buildup narrows the arteries that supply blood to the heart muscle, reducing oxygen delivery and raising the risk of angina and heart attack.
What causes coronary artery disease?
CAD is primarily caused by atherosclerosis, which develops when cholesterol and fatty deposits accumulate inside artery walls and are worsened by risk factors such as high blood pressure, smoking, diabetes, and unhealthy diet.
What are the early symptoms of coronary artery disease?
Common early symptoms include chest pain or pressure (especially with exertion), shortness of breath, fatigue, and discomfort in the arm, neck, or jaw, although some people have no symptoms until a heart attack occurs.
Can coronary artery disease be reversed?
While plaque buildup cannot always be completely reversed, lifestyle changes and medications can stabilize plaques, slow disease progression, and improve heart health, reducing the risk of heart attack.
How can I reduce my risk of coronary artery disease?
Maintaining a healthy diet, exercising regularly, managing blood pressure and cholesterol, quitting smoking, managing diabetes, and attending routine medical checkups significantly reduce risk.
Final Thoughts
Coronary artery disease is one of the most common cardiovascular conditions worldwide, but many cases can be prevented or controlled through early detection and heart-healthy choices. Understanding how plaque buildup affects coronary arteries, recognizing early warning signs, and following evidence-based prevention strategies can significantly lower the risk of heart attack and other cardiovascular complications. Working closely with healthcare professionals and maintaining consistent heart-healthy habits remain the most effective ways to protect long-term cardiovascular health.
⚠️ Medical Disclaimer
The information provided on MedEduHub is for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. If you experience chest pain, shortness of breath, sudden weakness, or symptoms of a possible heart attack, seek emergency medical care immediately. Always consult a licensed healthcare provider before making changes to your medical care plan.
Written by: Eden Grace Ramos, RN
Sources: this article draws on current evidence from the World Health Organization cardiovascular disease fact sheet, CDC heart disease and risk factor resources, American Heart Association coronary artery disease and cholesterol information, and National Heart, Lung, and Blood Institute materials on coronary heart disease and atherosclerosis.

