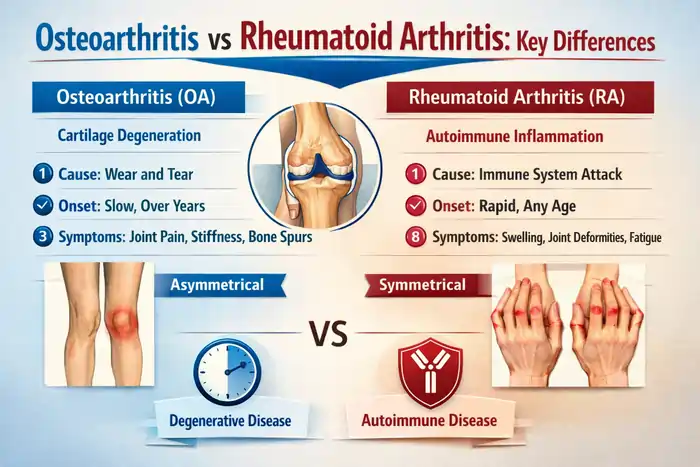
Osteoarthritis and rheumatoid arthritis are two of the most common forms of arthritis, but they are fundamentally different conditions in terms of cause, pattern, and long-term impact, as highlighted in clinical comparisons of osteoarthritis versus rheumatoid arthritis. Osteoarthritis (OA) is a degenerative joint disease caused by cartilage breakdown and mechanical wear over time, while rheumatoid arthritis (RA) is an autoimmune disorder in which the immune system mistakenly attacks the joints and triggers chronic inflammation.
Understanding osteoarthritis vs rheumatoid arthritis is critical because their causes, symptoms, diagnosis, and treatment approaches are not the same, a point underscored in detailed reviews of similarities and differences between OA and RA. If you need a broader overview of arthritis types and long-term management, you can explore our comprehensive pillar guide on chronic arthritis and long-term joint health.
What Is Osteoarthritis?
Osteoarthritis is the most common type of arthritis and is often described as a degenerative “wear-and-tear” joint disease, a description echoed in patient resources on osteoarthritis as a degenerative joint disorder. It develops gradually as cartilage cushioning the ends of bones breaks down and the entire joint structure begins to change.
Cartilage acts as a shock absorber in joints, and when it deteriorates, bones start to rub against each other, causing:
- Joint pain
- Stiffness
- Limited range of motion
- Bone spurs
- Joint space narrowing
Osteoarthritis most commonly affects:
- Knees
- Hips
- Hands
- Spine
It is considered a degenerative joint disease rather than an autoimmune condition, which is why clinical summaries often group OA under degenerative musculoskeletal disorders.
What Is Rheumatoid Arthritis?
Rheumatoid arthritis is a chronic inflammatory arthritis and a systemic autoimmune disorder. In RA, the immune system attacks the synovial membrane (the lining of joints), causing:
- Synovitis (inflammation of the joint lining)
- Swelling
- Warm joints
- Joint tenderness
- Progressive joint damage
This immune-driven process is described in depth in rheumatoid arthritis reviews from StatPearls and NIAMS.
Unlike osteoarthritis, RA is systemic and may also affect:
- Eyes
- Lungs
- Blood vessels
- Heart
Because rheumatoid arthritis is classified as inflammatory arthritis, it requires early treatment with disease-modifying medications, as emphasized in the American College of Rheumatology rheumatoid arthritis guidelines.
Main Differences Between Osteoarthritis and Rheumatoid Arthritis
Here is a clear comparison table for quick understanding:
| Feature | Osteoarthritis (OA) | Rheumatoid Arthritis (RA) |
|---|---|---|
| Cause | Cartilage degeneration and mechanical wear, described in degenerative OA overviews | Autoimmune inflammation where the immune system targets joints, as explained in RA pathophysiology resources |
| Type | Degenerative joint disease | Chronic inflammatory autoimmune disease |
| Onset | Gradual, over months to years | Can be rapid or subacute, sometimes with flares |
| Joint Pattern | Often asymmetrical, affecting one or a few weight-bearing joints | Typically symmetrical, especially in small joints of hands and feet |
| Morning Stiffness | Usually less than 30 minutes, improving quickly with movement | Often more than 60 minutes, improving slowly with activity |
| Systemic Symptoms | Rare systemic features | Common systemic symptoms such as fatigue and low-grade fever |
| Blood Tests | Usually normal inflammatory markers | RF and Anti-CCP may be positive, with elevated CRP and ESR in active disease |
| Treatment | Pain management, physical therapy, lifestyle changes, surgery if neededniams. | DMARDs, biologics, and targeted therapies following ACR/EULAR RA treatment recommendations |
Symptoms: How They Feel Different
Although both conditions cause joint pain and stiffness, their symptom patterns differ in ways that can help guide diagnosis, as shown in clinical comparisons of how OA and RA present in practice.
Osteoarthritis Symptoms
- Pain that worsens with activity or weight-bearing
- Stiffness after rest, often short-lived
- Crepitus (a grating or crackling sensation)
- Limited flexibility
- Mild to moderate swelling
Pain in osteoarthritis typically improves with rest and is closely linked to mechanical use of the joint, a pattern described in symptom-based OA guides.
Rheumatoid Arthritis Symptoms
- Persistent joint inflammation
- Warm, swollen joints
- Morning stiffness lasting more than one hour
- Fatigue and low energy
- Low-grade fever
- Symmetrical joint involvement (both sides of the body)
RA pain may persist even at rest because of ongoing inflammation, a hallmark highlighted in rheumatoid arthritis clinical overviews. If you’re unsure whether early joint symptoms may signal inflammatory disease, you can review our internal guide on early signs of arthritis and inflammatory joint disease.
Causes and Risk Factors
Osteoarthritis Risk Factors
Common risk factors for osteoarthritis include:
- Aging
- Obesity
- Joint injury
- Repetitive stress
- Genetic predisposition
Excess weight increases mechanical stress on knees and hips, a relationship described in osteoarthritis risk factor resources.
Rheumatoid Arthritis Risk Factors
Rheumatoid arthritis risk factors include:
- Genetic factors and family history
- Smoking
- Immune system dysfunction
- Hormonal influences
Unlike osteoarthritis, RA is not caused by joint wear, but by immune dysregulation, as shown in analyses of RA pathogenesis and risk factors.
Diagnosis: How Doctors Tell the Difference
Physical Examination
On physical exam, osteoarthritis often shows localized joint changes, bony enlargement, and pain with movement in specific joints. In contrast, rheumatoid arthritis often shows symmetrical swelling, tenderness of multiple small joints, and possible deformities in more advanced disease, as described in comparative exam findings for OA and RA.
Blood Tests
Rheumatoid arthritis may show:
- Positive rheumatoid factor (RF)
- Positive anti-CCP antibodies
- Elevated CRP and ESR
These immune and inflammatory markers are outlined in ACR-endorsed RA diagnostic criteria. Osteoarthritis usually does not elevate systemic inflammatory markers, and blood tests are often normal in isolated OA.
Imaging
Osteoarthritis imaging typically shows:
- Joint space narrowing
- Osteophytes (bone spurs)
- Subchondral bone changes
Rheumatoid arthritis imaging commonly reveals:
- Joint erosions
- Periarticular osteopenia
- Synovial inflammation and effusions
Radiologic differences are summarized in imaging-based comparisons of OA and RA. Early diagnosis is especially important in RA to prevent joint deformity and long-term disability.
Treatment Differences
For a full arthritis management overview that covers exercise, weight management, and multidisciplinary care, you can explore our main guide on chronic arthritis management and treatment strategies.
Osteoarthritis Treatment
Common osteoarthritis treatment options include:
- NSAIDs and other pain relievers
- Physical therapy and targeted exercises
- Weight management
- Joint injections (such as corticosteroids or viscosupplementation)
- Joint replacement surgery for advanced disease
These strategies are consistent with patient guidance from the Arthritis Foundation’s osteoarthritis management resources. For more detailed pain control strategies across chronic joint conditions, visit our internal article on treatment options for chronic joint pain.
Rheumatoid Arthritis Treatment
Rheumatoid arthritis treatment commonly involves:
- Conventional synthetic DMARDs (such as methotrexate)
- Biologic therapies (such as TNF inhibitors)
- Targeted synthetic DMARDs (such as JAK inhibitors)
- Short-term corticosteroids as needed
- Immunomodulatory regimens tailored to disease severity
RA treatment aims to control immune activity, reduce inflammation, and prevent joint damage, as outlined in the 2021 American College of Rheumatology RA treatment guideline. Practical summaries of these recommendations are available in Arthritis Foundation discussions of RA treatment guidelines.
Which Condition Is More Serious?
Rheumatoid arthritis is generally considered more serious due to systemic inflammation, risk of organ involvement, and increased cardiovascular risk, a point emphasized in long-term outcome comparisons of OA and RA. However, severe osteoarthritis can also cause significant disability, chronic pain, and loss of independence, especially when large weight-bearing joints are involved.
Can You Have Both?
Yes. Some individuals may develop both degenerative and inflammatory arthritis, particularly older adults with age-related OA and coexisting autoimmune RA, a pattern occasionally noted in clinical series comparing OA and RA features.
Long-Term Outlook
Osteoarthritis often progresses slowly and is managed symptomatically with pain control, exercise, and sometimes surgery, as described in NIAMS osteoarthritis prognosis summaries. Rheumatoid arthritis may progress more aggressively but can enter remission or low disease activity with early, aggressive DMARD therapy following treat-to-target RA management recommendations.
When to See a Doctor
Seek evaluation if you experience:
- Persistent joint swelling
- Severe morning stiffness
- Symmetrical joint pain
- Sudden worsening pain or loss of function
Early medical intervention improves outcomes in both OA and RA, and rheumatology societies stress timely referral in their guidance on early inflammatory arthritis.
Frequently Asked Questions
Is osteoarthritis worse than rheumatoid arthritis?
They are different conditions rather than “worse” or “better.” RA is more systemic and potentially more serious due to organ involvement and faster joint damage, as noted in comparative arthritis discussions.
Does rheumatoid arthritis shorten life expectancy?
Uncontrolled RA may increase cardiovascular risk and overall morbidity, but modern DMARD and biologic therapy recommended in ACR and EULAR RA guidelines has improved long-term outcomes substantially.
Can osteoarthritis turn into rheumatoid arthritis?
No. They are separate conditions with different mechanisms, which is clearly stated in educational materials on why osteoarthritis cannot turn into RA. However, an individual can coincidentally have both disorders.
Medical Disclaimer
The information provided on MedEduHub is for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. If you are experiencing severe joint swelling, fever, sudden immobility, or signs of a medical emergency, seek immediate medical attention or contact emergency services. Always consult your healthcare provider before starting or changing any treatment plan.
Written by: Eden Grace Ramos-Arsenio, RN
Medical Sources & References
This article is based on current clinical guidelines and peer-reviewed research from leading organizations, including the World Health Organization (WHO) musculoskeletal health fact sheets, the Centers for Disease Control and Prevention arthritis program, National Institutes of Health resources on osteoarthritis and rheumatoid arthritis, the American College of Rheumatology rheumatoid arthritis guidelines, and American Heart Association discussions of inflammation and cardiovascular risk.

